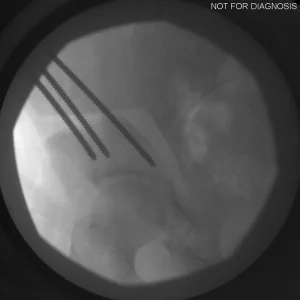
Procedure Overview
What Is a Periacetabular Osteotomy?
A periacetabular osteotomy (PAO) is a surgical procedure used to treat hip dysplasia, a condition in which the hip socket (acetabulum) does not adequately cover the ball of the hip joint (femoral head). Poor coverage can lead to pain, instability, and early arthritis.
During a PAO, the surgeon carefully cuts the bone around the hip socket and repositions it to provide better coverage of the femoral head. The socket is then fixed in its new position using screws. The goal is to improve hip stability, reduce pain, and preserve the patient’s natural hip joint.
Why Might a PAO Be Recommended?
PAO may be recommended if you:
- Have symptomatic hip dysplasia
- Experience hip or groin pain that limits activity
- Have minimal to no advanced arthritis in the hip
- Have a well-preserved hip joint but abnormal socket alignment
- PAO is most commonly performed in adolescents and young adults, but selected older patients may also benefit.
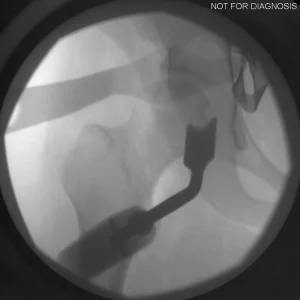
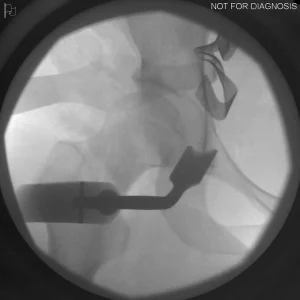
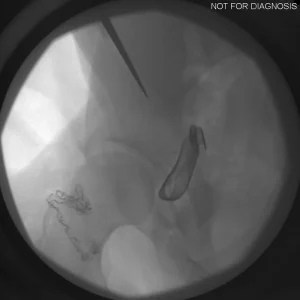
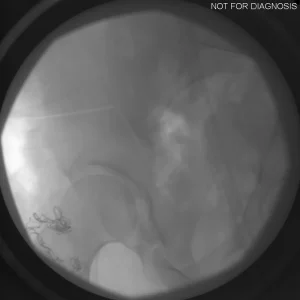
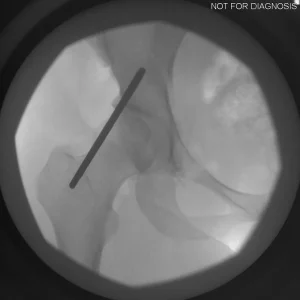
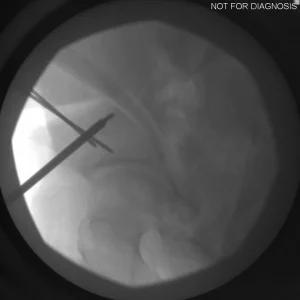
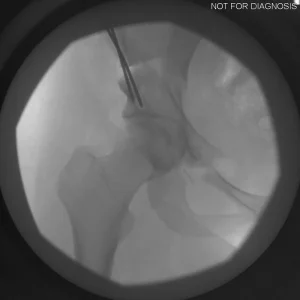
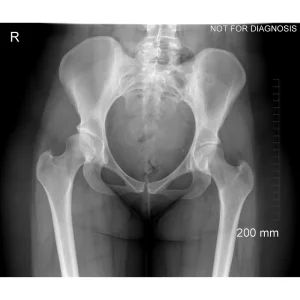
Understanding Hip Dysplasia (Imaging Explanation)
Hip dysplasia occurs when the hip socket does not fully cover the ball of the hip joint. This can be understood using imaging studies such as X-rays, CT scans, or MRI.
Labeled Imaging Diagrams (Conceptual)
Diagram 1: Normal Hip Anatomy
- Femoral head (ball) is well covered by the acetabulum (socket)
- Even distribution of load across the joint
- Reduced risk of cartilage wear
Diagram 2: Hip Dysplasia
- Shallow acetabulum with reduced coverage of the femoral head
- Increased stress on the edge of the joint
- Higher risk of pain, labral tears, and early arthritis
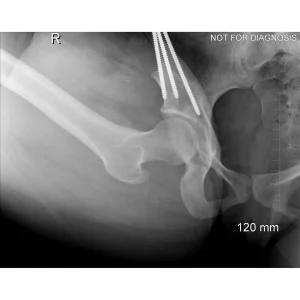
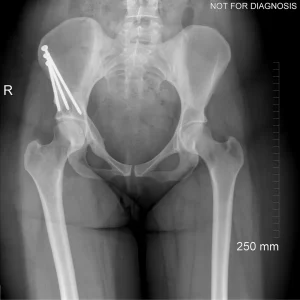
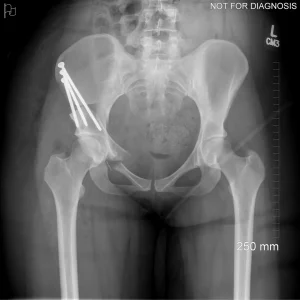
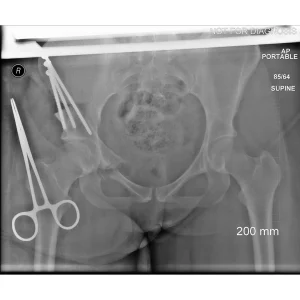
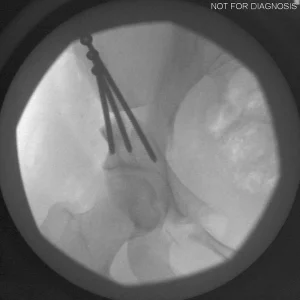
- Diagram 3: Hip After Periacetabular Osteotomy (PAO)
Diagram 3: Hip After Periacetabular Osteotomy (PAO)
- Acetabulum repositioned to improve femoral head coverage
- Load more evenly distributed across the joint
- Screws shown securing the acetabulum in its new position
These diagrams are commonly used in clinic to help patients visualize the problem and understand how PAO corrects hip mechanics. Dr Grammatopoulos will review your X-rays alongside these illustrations to explain your individual anatomy and surgical plan.
Long-Term Outcomes
- Most patients experience significant pain relief and improved hip function after PAO.
- When performed before advanced arthritis develops, PAO can significantly delay or prevent the need for hip replacement.
Clinical Outcomes & Patient Safety
Key Benefits
- Preserves your natural hip joint
- Improves hip stability and joint mechanics
- Reduces pain and improves function
- May delay or prevent the need for a total hip replacement
Risks & Considerations
- Infection
- Blood clots
- Nerve or blood vessel injury
- Blood loss (transfusion may be required)
- Fracture of the pelvic bones
- Delayed bone healing
- Ongoing pain or stiffness
- Progression to hip arthritis requiring future hip replacement
Surgical Approaches
PAO (Periacetabular Osteotomy)
- Preserves your own hip joint
- Best for younger patients with little or no arthritis
- Longer and more demanding recovery
- Aims to delay or avoid hip replacement
Total Hip Replacement
- Replaces the hip joint with artificial components
- Best for patients with advanced arthritis
- Faster early recovery
- Implants may wear out over time and may require revision
PAO Compared With Total Hip Replacement
| Feature | PAO (Periacetabular Osteotomy) | Total Hip Replacement |
|---|---|---|
| Joint preserved | Yes | No |
| Best age group | Young adults | Middle-aged & older adults |
| Arthritis present | Minimal | Moderate to severe |
| Recovery time | Longer | Shorter |
| Implant lifespan | Not applicable | 15–25+ years |
The Surgery
- PAO surgery typically takes 2-4 hours
- It is performed under general anesthesia
- Several controlled bone cuts are made around the hip socket
- The socket is repositioned and fixed with screws
- The hip joint itself is preserved
Preparing for Surgery
Medical Preparation
- Attending a preoperative assessment clinic to review your overall health. This may require blood tests, X-rays, and heart tests.
- Reviewing medications with your healthcare provider, as some may need to be stopped before surgery.
- Managing existing conditions (such as diabetes, anemia, high blood pressure, or heart disease) as well as possible
- Treating existing infections (including dental, skin, or urinary infections) before surgery
Lifestyle Preparation
- Stop smoking, ideally several weeks before surgery, as smoking can delay healing and increase risk of complications
- Maintain a healthy diet rich in protein, vitamins, and minerals, including adequate calcium and vitamin D, to support healing
- Begin/continue preoperative exercises ("prehabilitation") to strengthen hip and leg muscles and improve flexibility
Plan Ahead
- Arrange time off work or school (often several months)
- Organize help at home after surgery. You will be limited weight bearing for 6-8 weeks.
- Plan transportation to and from the hospital on the day of surgery and for follow-up appointments. You will not be able to drive initially.
- Prepare questions and concerns to discuss with your surgical team
What to Expect After Surgery
 Recovery In Hospital
Recovery In Hospital
- Most patients stay in the hospital for 0–5 days.
- Pain will be managed with medications
- You will begin physiotherapy in hospital
- Weight-bearing is limited and crutches or a walker are required
- Blood-thinning medication and compression devices may be used to reduce the risk of blood clots
- Nurses and therapists will teach you how to move safely, get in and out of bed, dress, and use the bathroom
 Recovery At Home
Recovery At Home
Recovery at Home
Preparing your home before surgery can help make your recovery smoother and more comfortable.
Upon your return home, you can expect:
- Partial or non–weight bearing for 6–8 weeks
- Physiotherapy continues for several months
- Swelling, stiffness, and fatigue are common during recovery
- Gradual progression of activity is essential for bone healing
Screw Removal
In most cases, the screws are left in place. However, if they cause irritation, removal can be considered after the bone has healed, which is typically 9-12 months after the initial PAO.
Return to Work, Driving & Sports
 Return to Work
Return to Work
- Desk-based work or school: often 8–12 weeks
- Physically demanding work: several months, depending on your recovery
 Driving
Driving
- You are no longer taking narcotic pain medication
- You can safely control the vehicle and perform an emergency stop
- Your surgeon confirms it is safe
 Sports
Sports
- Running and impact sports are usually delayed for at least 6–12 months
- Final clearance depends on healing and surgeon guidance
Frequently Asked Questions
Will I need a hip replacement in the future?
Some patients may still need a hip replacement later in life, but PAO often delays this by many years.
Is recovery longer than a hip replacement?
Yes. Recovery after PAO is typically longer and more demanding because bone healing is required.