Procedure Overview
What is a Total Hip Replacement?
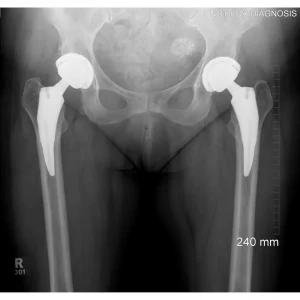
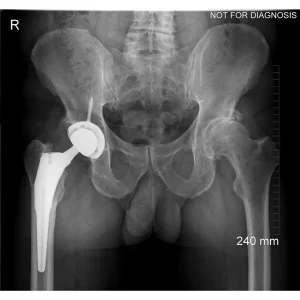
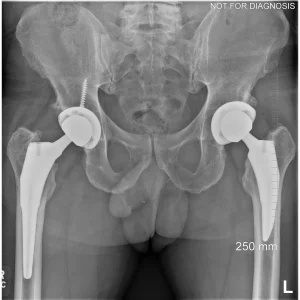
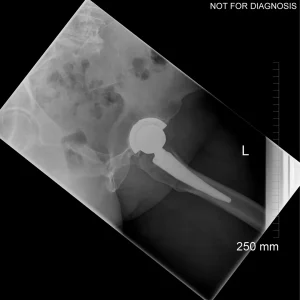
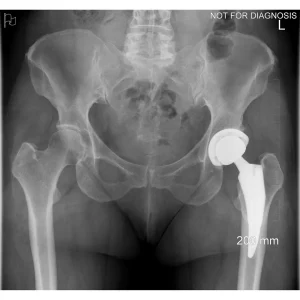
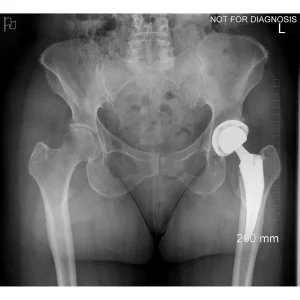
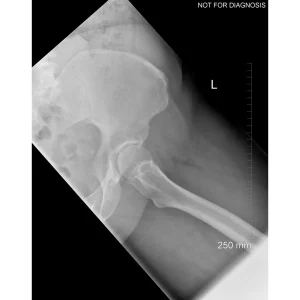
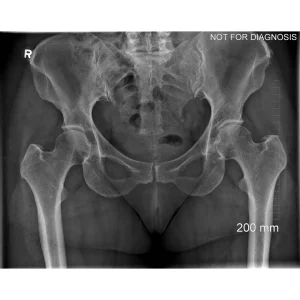
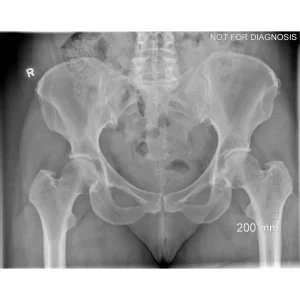
A total hip replacement (also called total hip arthroplasty) is a surgical procedure in which a damaged or worn hip joint is replaced with artificial components. The hip is a ball-and-socket joint, meaning the ball at the top of the thigh bone sits in a socket on the pelvis. During surgery, the damaged ball (femoral head) is replaced with a metal or ceramic ball attached to a stem, and the damaged socket is replaced with a metal cup lined with plastic, ceramic, or metal.
The goal of hip replacement surgery is to relieve pain, improve mobility, and enhance quality of life.
Why Might I Need a Hip Replacement?
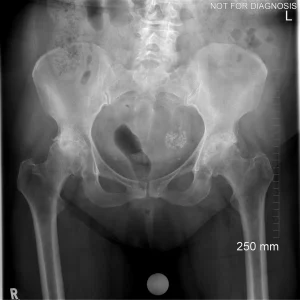
You may be advised to have a total hip replacement if you have:
- Severe hip pain that limits daily activities (walking, climbing stairs, getting dressed)
- Pain that persists despite medications, physiotherapy, or injections
- Stiffness or loss of movement in the hip
Hip damage caused by conditions such as:
- Osteoarthritis (most common)
- Rheumatoid arthritis
- Avascular necrosis (loss of blood supply to the hip bone)
- Hip fracture or trauma
- Congenital or developmental hip disorders
Clinical Outcomes & Patient Safety
Key Benefits
- Significant reduction or elimination of hip pain
- Improved movement and function
- Increased independence in daily activities
- Improved sleep and overall quality of life
Risks & Considerations
- Infection
- Blood clots in the legs or lungs
- Nerve or blood vessel injury.
- Dislocation of the new hip joint.
- Difference in leg length.
- Fracture of surrounding bone.
- Loosening or wear of the prosthesis over time.
- Ongoing pain or stiffness (rare).
- Medical-related complication (e.g. urinary tract infection, pneumonia).
Surgical Approaches
Anterior Approach Preferred
- Incision is made along the front of the hip
- Muscles are spread rather than cut
- May allow faster early recovery and fewer movement restrictions
- Not suitable for all patients and requires specialized equipment and training
Posterior Approach Preferred
- Incision is made on the side of the hip
- Provides excellent visibility of the hip joint
- Widely used and well-studied
- Slightly higher risk of dislocation early after surgery
- Certain movement precautions may be recommended initially (such as avoiding deep bending or twisting) to aid healing of cut muscles.
Lateral Approach (Least commonly used)
- Incision is made on the side of the hip
- Commonly used in Canadian centres but it is not common at The Ottawa Hospital due to significant muscle trauma associated.
- Lower risk of dislocation
- Some patients may experience temporary weakness of the hip abductor muscles, which usually improves with physiotherapy
What This Means For You
- Long-term outcomes are similar regardless of approach
- Recovery instructions and precautions may differ depending on the approach used
- Your surgeon will discuss which approach is planned and what specific precautions you should follow
The Surgery
- Total hip replacement usually takes 1–2 hours
- It is performed under general or spinal anesthesia
- The surgeon removes the damaged bone and cartilage and inserts the artificial joint
- The incision is then closed with sutures or staples
Preparing for Surgery
Good preparation before surgery can improve recovery and reduce complications.
Your healthcare team will guide you, but general recommendations include:
Medical Preparation
- Attending a preoperative assessment clinic to review your overall health. This may require blood tests, X-rays, and heart tests.
- Reviewing medications with your healthcare provider, as some may need to be stopped before surgery.
- Managing existing conditions (such as diabetes, anemia, high blood pressure, or heart disease) as well as possible
- Treating existing infections (including dental, skin, or urinary infections) before surgery
Lifestyle Preparation
- Stop smoking, ideally several weeks before surgery, as smoking can delay healing and increase risk of complications
- Maintain a healthy diet rich in protein, vitamins, and minerals to support healing
- If advised, try to lose excess weight to reduce stress on the new joint
- Begin preoperative exercises ("prehabilitation") to strengthen hip and leg muscles and improve flexibility
Plan Ahead
- Arrange time off work and discuss return-to-work plans with your healthcare provider
- Organize help at home for the first few weeks after surgery
- Plan transportation to and from the hospital on the day of surgery and for follow-up appointments. You will not be able to drive initially.
- Prepare questions and concerns to discuss with your surgical team
What to Expect After Surgery
 Recovery In Hospital
Recovery In Hospital
- Most patients stay in hospital for 0-2 days.
- Pain will be managed with medications.
- You will stand and begin walking with assistance (walker/crutches) immediately.
- Physiotherapy starts early to restore movement.
- Blood-thinning medication may be used to reduce clot risk.
 Recovery At Home
Recovery At Home
- Continue prescribed physiotherapy exercises daily.
- Gradually increase walking and activity as advised.
- Use walking aids until your surgeon says they are no longer needed.
- Experience mild to moderate pain and swelling (common for several weeks).
- Avoid certain movements to reduce dislocation risk.
- Keep the surgical wound clean and dry.
Return to Work, Driving & Sports
 Return to Work
Return to Work
- Sedentary work: 4–6 weeks
- Light physical work: 6–8 weeks
- Heavy manual labour: 8–12 weeks+
 Driving
Driving
- You are no longer taking narcotic pain medication
- You can safely control the vehicle and perform an emergency stop
- Your surgeon confirms it is safe
 Sports
Sports
- Walking
- Swimming
- Cycling
- Lower-impact fitness programs
Implant Longevity & Dental Advisory
 Implant Longevity
Implant Longevity
- Age at the time of surgery
- Activity level and type of activities performed
- Body weight
- Bone quality
- Surgical technique and implant type
 Dental & Antibiotics
Dental & Antibiotics
- Patients should not be exposed to the adverse effects of antibiotics when there is no evidence that such prophylaxis is of any benefit.
- Routine antibiotic prophylaxis is not indicated for dental patients with total joint replacements, nor for patients with orthopedic pins, plates and screws.
- Patients should be in optimal oral health prior to having total joint replacement and should maintain good oral hygiene and oral health following surgery. Orofacial infections in all patients, including those with total joint prostheses, should be treated to eliminate the source of infection and prevent its spread.
- Have a weakened immune system
- Have poorly controlled diabetes
- Have had previous joint infections
- Are undergoing invasive dental procedures involving significant gum manipulation
Frequently Asked Questions
What is a Total Hip Replacement?
A total hip replacement (also called total hip arthroplasty) is a surgical procedure in which a damaged or worn hip joint is replaced with artificial components. The hip is a ball-and-socket joint, meaning the ball at the top of the thigh bone sits in a socket on the pelvis. During surgery, the damaged ball (femoral head) is replaced with a metal or ceramic ball attached to a stem, and the damaged socket is replaced with a metal cup lined with plastic, ceramic, or metal.
The goal of hip replacement surgery is to relieve pain, improve mobility, and enhance quality of life.
Why Might I Need a Hip Replacement?
You may be advised to have a total hip replacement if you have:
Severe hip pain that limits daily activities (walking, climbing stairs, getting dressed)
Pain that persists despite medications, physiotherapy, or injections
Stiffness or loss of movement in the hip
Hip damage caused by conditions such as:
Osteoarthritis (most common)
Rheumatoid arthritis
Avascular necrosis (loss of blood supply to the hip bone)
Hip fracture or trauma
Congenital or developmental hip disorders
Will my hip replacement limit my movement?
Most patients experience improved movement compared to before surgery. Some movements may feel different, but everyday activities usually become much easier once healing is complete.
Can I kneel or bend after hip replacement?
Kneeling and bending are often possible after recovery, but comfort varies between individuals. Your physiotherapist can guide you on safe techniques.
Will I have a scar?
Yes. You will have a scar where the incision was made. Over time, it usually fades and becomes less noticeable.
Can my hip replacement get infected years later?
Although rare, infections can occur at any time if bacteria enter the bloodstream. Maintaining good dental hygiene, treating infections promptly, and following medical advice help reduce this risk.
Will I set off metal detectors at airports?
Most hip replacements contain metal, but they rarely trigger airport metal detectors. You do not need a special card. If asked, simply inform security staff that you have a hip replacement.
How Long Will a Hip Replacement Last?
Modern hip replacements are designed to be durable and long-lasting.
Approximately 90–95% of hip replacements are still functioning well at 10 years
About 80–85% last 20 years or longer
How long a hip replacement lasts depends on several factors, including:
Age at the time of surgery
Activity level and type of activities performed
Body weight
Bone quality
Surgical technique and implant type
High-impact activities (such as running or jumping sports) and excessive wear over time may shorten the lifespan of the implant. Low-impact activities such as walking, swimming, cycling, and golf are generally encouraged.
If a hip replacement wears out or loosens, a revision surgery may be required. However, advances in materials and surgical techniques continue to improve implant longevity.